by Emma Pickett IBCLC
Concerns that they are struggling with low milk supply are often cited by UK mothers as a reason for cessation of breastfeeding and certainly cessation of exclusive breastfeeding1.
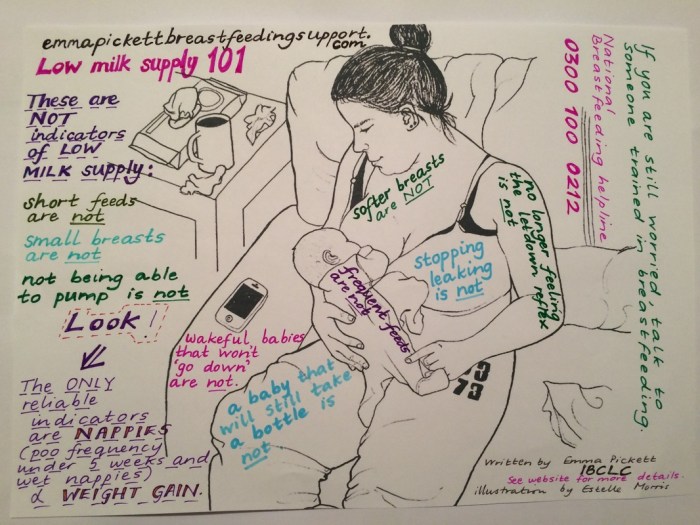
However not all mothers who worry about low milk supply have an actual issue. Perception of low milk supply is a common problem when parents misinterpret normal newborn behaviour (such as cluster feeding, growth spurts and frequent feeding in a newborn) or misunderstand how breastfeeding works (not appreciating that breasts may come to feel softer as weeks go by, a baby’s swallowing pattern may change as the fat content of breastmilk milk rises or that response to a breast pump is not a measurement of milk supply).
When a mother fears low milk supply and begins supplementation, this may then lead to an actual decrease in her milk production.
In some cases there is an insufficient milk intake, as indicated by inadequate weight gain and insufficient stooling under 5 weeks. In the majority of cases this will be initially due to the quality of milk transfer (though over time, poor quality milk transfer will impact on milk production.)
Fears about low milk supply, whether due to perception or reality, can erode a mother’s confidence and cause on-going distress. Effective support may enable a mother to accept normal breastfeeding patterns and move forward with greater confidence or correct issues with milk transfer and adjust her milk production.
In rare cases, where mothers have a primary issue with lactation, more specialist help may be required to investigate the underlying issues.
An Issue with Milk Transfer
- Is the mother breastfeeding regularly enough?
- Is she feeding in response to baby’s cues ie. not trying to impose a ‘routine’?
- or alternatively is the baby sleepy and jaundiced and she is waiting for cues which could cause insufficient feeds?
- Is she staying on one breast for extended periods beyond the point the baby is effectively transferring milk and milk volume needs to be increased with some ‘switch nursing’ (using other side)?
- Or is she removing the baby from the breast prematurely and reducing the amount of higher fat content milk the baby receives?
- How is the POSITIONING and ATTACHMENT (latching)
- Is the mother comfortable? (not just nipples but mother’s back/ arms)
- Is the nipple misshaping after a feeds? (suggesting it’s being pressed incorrectly against the hard palate or against the rear of the tongue)
- Does the nipple come out looking blanched because of compression?
- Is there visible nipple damage?
- Does the mother experience blocked ducts and mastitis (suggesting ineffective milk transfer)?
- Could there be an issue with the baby’s anatomy?
- Tongue-Tie? (which may not be immediately visible and doesn’t have to mean a frenulum at the tip of baby’s tongue)
- Asymmetry
- High palate
- Low tone
An Issue with Lactation
- In rarer cases, there may be issues with the mother’s primary ability to lactate. Figures vary but based on breastfeeding figures in comparable countries, we can suppose approximately 2-5% of women have underlying issues that may affect milk production and milk transfer2, 3. Multiple factors may account for this, for example:
- This could be due to a history of breast surgery or breast injury,
- PCOS (a 1/3 of mums with PCOS will experience supply problems)
- Other hormonal issues (e.g. retained placenta, theca lutein cysts, thyroid conditions)
- Insufficient glandular tissue/hypoplasia (breasts may be tubular, widely-spaced, not developing in puberty, not changing in pregnancy, mother not experiencing breast changes after birth)
- or significant blood loss in delivery (without sufficient transfusion causing pituitary compromise).
- Is the mother taking hormonal contraceptives? Both Combined Hormonal Contraception and Progesterone Only Contraception (POP/LARC) may affect supply in some women.
Remember: A baby may also have underlying health issues which affect weight gain.
How Would we Help a Mother who Describes Low Milk Supply?
- Has anyone observed her feeds? Who observed and when? Where could she go to have her feeds properly observed?
- Has she had information about what is normal in the first few weeks of breastfeeding and newborn care?
- Could she use expressing/pumping to stimulate supply? Double hospital grade pumping is ideal (eg. renting from a local NCT pump agent or national pump hire company). Pumping after applying warm compresses and breast massage, using hand expression at the end of a feed or to help stimulate the milk ejection reflex.
- We need to monitor weight but bear in mind overweighing may not be helpful and could affect maternal confidence.
- The mother can gain reassurance from monitoring nappies, but stooling rate over 5 weeks is not a reliable indicator of milk transfer and as a baby receives more breastmilk, their stooling rate may actually decrease.
- Look at bottlefeeding technique if top-ups are being used. Does the bottle shape and position encourage a wide latch that mimics a breastfeeding gape? In some cases, ‘paced bottlefeeding’ may be encouraged (though caution advised if baby’s weight gain is a serious concern and higher flow feeds may be needed).
- Could the mother use an Supplemental Nursing System (SNS) to give supplements at the breast? (this could be made using a 5 French feeding tube)
- Help her to understand that supplementation may make a baby healthier/ stronger/more effective at the breast and can support breastfeeding (rather than being ‘failure’). That supplementation isn’t simply ‘getting a baby to put on weight so it looks better on a chart’ but helping to make a baby a better breastfeeder. However she also needs to understand the relationship between the quantity of supplementation and her own supply.
- Encourage her to reflect on her support network. Have her family and friends faded away now they perceive the newborn phase to be over? The next two weeks may be particularly crucial if a mum is going to focus on developing her supply.
- Consider testing thyroid function in mothers with low milk supply
- Consider the use of galactagogues.
With thanks to Emma for her contribution to this website. Her own website Emma Pickett Breastfeeding Support can be found here.
Further Information
Global Health Media Project: Breastfeeding Series Not Enough Milk Video
Breastfeeding After Breast and Nipple Surgeries (BFAR)
NICE CKS Breastfeeding Problems Last Revised May 2017
References
- UK Infant Feeding Survey (2010)
- Australian Government Department of Health: Norway -The WHO Code and Breastfeeding: An International Comparative Overview Updated May 2012 – Includes data on breastfeeding rates in Norway which can be compared to those in the UK.
- OECD Family database: OECD- Social Policy Division- Directorate of Employment, Labour and Social Affairs, CO1.5: Breastfeeding Rates Updated October 2009 – Includes breastfeeding rates in Hungary and other OECD countries which can be compared to those in the UK.

You must be logged in to post a comment.