by Dr Louise Santhanam, General Practitioner
My GP could help me most by listening to my feelings, and signposting me to good support.
LR, Mother
My GP could help me most by admitting he is not a lactation expert and referring me to one when needed.
SB, Mother
Why is Breastfeeding Support Necessary?
Results from the 2010 UK Infant Feeding Survey demonstrated that while almost 70% of mothers were exclusively breastfeeding at birth, this figure had dropped to 23% by 6 weeks postnatal1.
- 80% of mothers who stopped breastfeeding within the first week reported they would have like to continue for longer.
- 85% of mothers who had stopped breastfeeding between one and two weeks reported they would have like to continue for longer.
- 63% of mothers who had stopped breastfeeding by 8-10 months reported that they would have liked to continue for longer.
Many women who initiate breastfeeding stop before they had planned to do so due to problems with attachment at the breast (the ‘latch’), problems with milk supply (real or perceived) and pain. Mothers who stop breastfeeding in the first week report that an easier ‘latch’, less pain and more support and guidance from hospital staff, midwives and family could have helped them to continue to breastfeed1.
 A significant proportion of breastfeeding problems can be managed with the help of experienced breastfeeding supporters, and many problems require attention to positioning and attachment at the breast, which, once managed can improve milk supply due to more effective milk transfer, and reduce nipple pain.
A significant proportion of breastfeeding problems can be managed with the help of experienced breastfeeding supporters, and many problems require attention to positioning and attachment at the breast, which, once managed can improve milk supply due to more effective milk transfer, and reduce nipple pain.
Achieving one’s goals for duration of breastfeeding has been shown to reduce the risk of postnatal depression, while mothers who plan to breastfeed but do not go on to do so are at higher risk2. Higher depression scores have been demonstrated in mothers who stop breastfeeding due to physical difficulty and pain, rather than personal choice3. A recent study demonstrated that the quality of breastfeeding support is also important for maternal mental health4. Among women with breastfeeding difficulties, those who did not report a negative breastfeeding support experience were at decreased risk of postpartum depression.
Messages which promote breastfeeding need to be accompanied by support from healthcare professionals, family and friends, and society in general. The responsibility for healthy infant feeding should be viewed as a collective one, rather than that of an individual with the potential for personal ‘failure’5. In recognition of this, for World Breastfeeding Week August 2016, GPIFN was a joint signatory to the Unicef UK Baby Friendly Initiative Call to Action, calling on the Government to work to create a supportive, enabling environment for women who want to breastfeed in the UK.
Multifactoral determinants of breastfeeding need supportive measures at many levels, from legal and policy directives to social attitudes and values, women’s work and employment conditions, and heath-care services to enable women to breastfeed. When relevant interventions are delivered adequately, breastfeeding practices are responsive and can improve rapidly.
Rollins N.C. et al (2016) The Lancet Breastfeeding Series
Breastfeeding Support Colleagues
Most GPs will be familiar with a Midwife or Health Visitor giving advice on infant feeding and breastfeeding support. Midwifery and Health Visiting training includes focus on these topics but, similarly to medicine, cover a broad range of topics. Many Midwives and Health Visitors are very skilled at breastfeeding support, having trained with one of the voluntary Breastfeeding Support organisations, undertaken further training to serve as locality Infant Feeding Leads, or achieved IBCLC qualification (see below). However, others may not have had extensive training in infant feeding support and if feeding problems for a mother persist in the community, the GP may need to refer to colleagues who have specialist expertise in lactation management.
The following information offers explanation of some of the roles linked to infant feeding that may be less familiar to GPs.
The following Table from LCGB covers the roles of:
- International Board Certified Lactation Consultant (IBCLC)
- Breastfeeding Counsellor
- Breastfeeding Supporter
- La Leche League Leader
- Breastfeeding Peer Supporter
- Other professionals working in a Baby Friendly Initative accredited setting
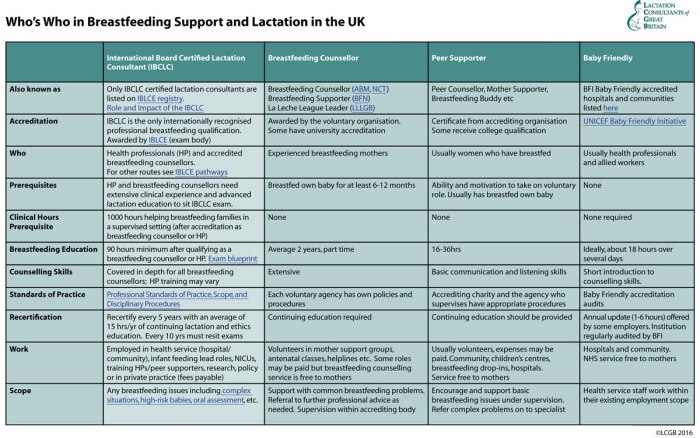
Breastfeeding Counsellors and Peer Supporters: will usually have trained with one of the four major UK organisations that provide voluntary breastfeeding support in the UK, or within the NHS.
‘Lactation Consultant’: this term alone is not protected in the UK and technically can be used by anyone, regardless of qualifications or experience. This is in contrast to those who have trained, passed the exam and registered with the International Board of Lactation Consultant Examiners who may use the title IBCLC (International Board Certified Lactation Consultant) and have an IBCLC certification number.
International Board Certified Lactation Consultant (IBCLC): An IBCLC is the professional qualified in the clinical management of breastfeeding and trained to deal with complex issues. IBCLCs are certified, registered and work within professional guidelines and codes set by the International Board of Lactation Consultant Examiners (IBLCE). In the UK the IBCLCs are not technically ‘registered healthcare professionals’ as defined by the Department of Health, but registered healthcare professionals such as Health Visitors and Midwives may be dual qualified as an IBCLC. IBCLCs use their specialist skills within the NHS including in service lead roles, infant feeding clinical education, and many deliver specialist services supporting mothers and babies with complex feeding situations. There are also IBCLCs working in private practice.
Tongue-Tie Practitioner: A practitioner competent in assessment of tongue-tie and tongue-tie division (frenulotomy). The role is limited to registered healthcare professionals as defined by the Department of Health in the UK and tongue-tie division should fall within the scope of practice for the individual performing it. Most commonly this role is performed by Doctors with relevant training and experience (usually Paediatric, ENT and Oral Surgeons) or Nurses, Health Visitors and Midwives with specialist training infant feeding. Some Dentists may also carry out the procedure. A Tongue-Tie Practitioner should also have advanced breastfeeding skills (preferably also holding the IBCLC qualification) or work alongside someone with advanced skills6.
Infant Feeding Lead (IFL): An NHS Trust’s or Health Board’s appointed lead for strategic issues around infant feeding and trust education. The IFL may be hospital based, and some areas also have a community IFL.
The National Infant Feeding Network (NIFN): The professional network for NHS Infant Feeding Leads across the UK. The NIFN is currently supported by the Unicef UK Baby Friendly Initiative.
Unicef Baby Friendly Initiative: Worldwide programme of the World Health Organization and Unicef to encourage maternity hospitals to implement the 10 Steps to Successful Breastfeeding and to practise in accordance with the International Code of Marketing of Breastmilk Substitutes.
Unicef UK Baby Friendly Initiative (BFI): Accredits UK health care settings according to achieving set standards. Hospitals and the Community may have a BFI Lead healthcare professional who is responsible for maintaining Baby Friendly Standards and accreditation/re-accreditation.
References
- UK National Infant Feeding Survey 2010
- Borra C, Iacovou M, Sevilla A. New Evidence on Breastfeeding and Postpartum Depression: The Importance of Understanding Women’s Intentions. Maternal and Child Health Journal. 2014;19(4):897-907.
- Brown A, Rance J, Bennett P. Understanding the relationship between breastfeeding and postnatal depression: the role of pain and physical difficulties. Journal of Advanced Nursing. 2015;72(2):273-282.
- Chaput K, Nettel-Aguirre A, Musto R, Adair C, Tough S. Breastfeeding difficulties and supports and risk of postpartum depression in a cohort of womenwho have given birth in Calgary: a prospective cohort study. Canadian Medical Association Journal Open. 2016;4(1):E103-E109.
- Ashmore S. Changing the conversation around breastfeeding 2016
- Association of Tongue Tie Practitioners: Tongue-Tie Training FAQs

You must be logged in to post a comment.